The Pandemic at Your Fingertips
Ten years ago, Christopher Carroll was serving as chief macroeconomist on the Obama Administration’s Council of Economic Advisers. The group was reviewing proposals for stimulus packages to repair the collapse in consumption spending caused by the Great Recession of 2007–08. (Crashes are most often caused by a collapse in consumption spending, not in the financial sector.)
But while there were 30 years’ worth of data on the “average” consumer, there was a gaping hole when it came to data on how actual consumers—many of whom have far less wealth or financial stability than the mythical typical one—would likely respond to a variety of possible measures.
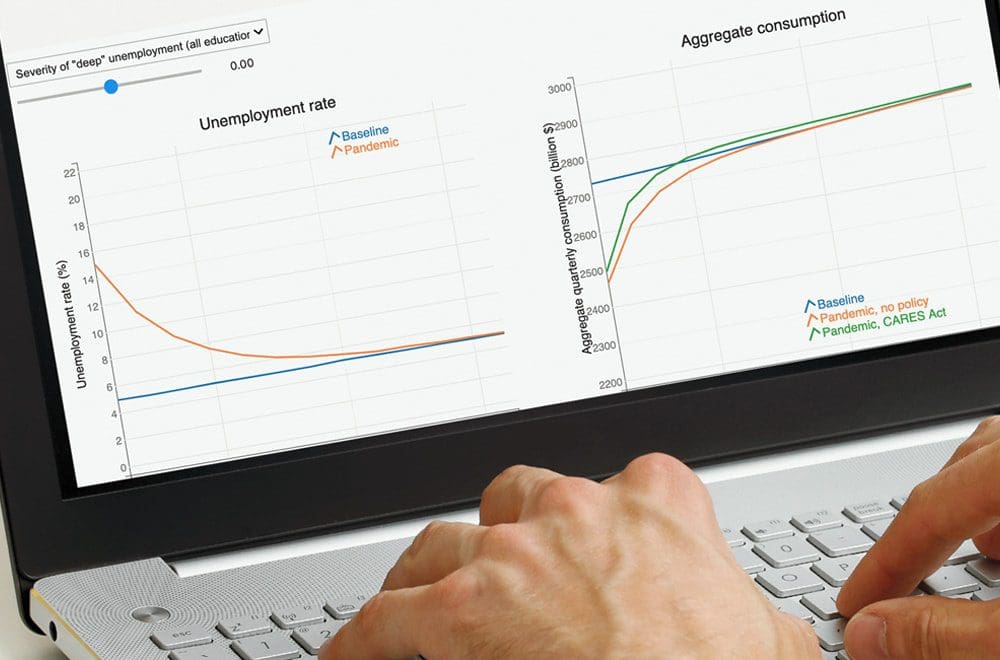
Fast forward to the spring of 2020 and the rapid onslaught of COVID-19, when an email popped up from the person in the Trump Administration now in Carroll’s former position. Did Carroll happen to have any tools to predict consumers’ responses to possible stimulus packages the council was considering in the face of the pandemic?
Conveniently, Carroll had spent the intervening decade creating just the tool he himself had wished for: a macroeconomic model that accounts for crucial microeconomics facts, like how many households have very little wealth, and the role that uncertainty plays in consumer decisions. It was on the verge of publication, and just in time to help inform the CARES Act passed by Congress in March.
“This time, there was a ready-built apparatus for assessing the consequences of different stimulus choices,” Carroll says of his model.
Drawing on complex mathematical techniques first used to calculate the trajectories for the Apollo spacecraft, Carroll and his colleagues developed a model that takes into account the reality that households will react differently to an influx of cash depending on their individual financial situations and perceptions of what uncertainty means for them. (“The mathematics of figuring out how to rationally behave in a world with lots of uncertainty is way harder than Apollo,” Carroll laughs.)

It was frustrating that there was no academic research that would really inform our projections of what the consequences would be of different stimulus policies.”
—Christopher Carroll, professor in the Department of Economics
The CARES Act sent a base dollar amount to individuals below a certain income, who would be likely to spend the extra cash—and tapered that amount the more an individual earned—because higher earners would more likely just park the windfall in savings. This tailored approach ensured a more effective use of the money to stimulate spending than a blanket payout would have done, Carroll says.
The model also incorporates the uncertainty element, acknowledging that some people you might expect to spend the cash would save it instead, worried about job loss and future prospects. In fact, May’s savings rate—typically around 7 percent—was a whopping 30 percent this year.
From the beginning, Carroll and his colleagues were interested in creating a user-friendly tool that people could manipulate themselves depending on their purposes. So they used a grant from the Sloan Foundation to hire technical help to allow users to download code and tweak it to adjust for various variables. One of the specialists suggested something much more entertaining, Carroll says: a dashboard with interactive sliders to model the economic response to the pandemic, with the ability to change the lockdown’s duration, the unemployment rate, and about two dozen other parameters. The dashboard is now free and available to the public; a tangible result of that decade he spent computing and modeling.
For fun, Carroll sent the dashboard to an old friend. The friend’s response: “It’s given me the godlike feeling that I can control the future of the pandemic. Now all I need is a button to cure COVID.”
Giving COVID-19 the Slip
Stephen Fried, an assistant professor in the Department of Chemistry, is helping lead a study that may hold a key to destroying not only SARS-CoV-2, the virus that causes COVID-19, but perhaps many other harmful viruses that infect humans.
Fried and his co-investigators from Arizona State University and Stony Brook University received a $150,000 grant from the Research Corporation for Science Advancement to study a specific part of the virus’s RNA called a slippery sequence. While he says the idea is too new to have an impact on the current pandemic, he hopes it might pave the way for a novel family of antiviral drugs that stop deadly viruses like SARS, MERS, and Zika from replicating in humans.

All cells require proteins to perform their functions. For human cells to create proteins, the DNA converts a gene into a strand of RNA—think of it as a protein purchase order—which is then sent to the ribosomes, the manufacturers of the cell. These ribosomes are designed to always read the full RNA strand and create the requested proteins, fulfilling the entire purchase order, so to speak.
Coronaviruses are RNA viruses, meaning they contain no DNA. This makes them similar to other viruses that are particularly dangerous for humans, such as the flu, Fried says. Once the coronavirus penetrates the human cell with its RNA, the ribosomes begin quickly producing virus proteins. But that reliance on RNA might also be the pathogen’s Achilles’ heel.
“If your genome is made out of DNA, you control your cells by basically only converting genes to RNA when you want certain proteins; and if you don’t want them, you just don’t convert the gene to RNA,” Fried says. “It’s like a complicated on-off switchboard. But if you’re a coronavirus, you can’t do that because your entire genetic code is in one long piece of RNA. By default, every gene is on, so every protein would be produced in equal amount.”
Genetically, having all genes “on” is bad for coronaviruses, because they don’t need equal amounts of all their proteins to function. Think of it as one gigantic purchase order with every protein ever needed in the virus’s life cycle produced at once—that would be chaotic and inefficient, Fried says. To survive and thrive, the virus must find a way to force the host cell’s ribosomes to stop reading its RNA and producing proteins from time to time. To do this, it includes in its RNA strand what’s called a slippery sequence. About 90 percent of the time, when the human ribosome encounters that slippery sequence, it stops reading and halts protein production. The remaining 10 percent of the time, the ribosome slips through, reading the entire RNA strand and producing the remaining proteins.

The reason we’re so excited about this idea is because during this slipping of the ribosome, the virus is actually at the mercy of our cells.”
—Stephen Fried, assistant professor in the Department of Chemistry
“That’s where our idea comes in,” Fried says. “What if there were a way to basically prevent all ribosomes from slipping past that slippery sequence? It would be game over for the virus because replicase—the enzyme that causes RNA to replicate itself—is actually located after the slippery sequence in the virus RNA strand.”
Fried and his co-investigators are currently “playing” with DNA to create the elements needed to test their idea and eventually engineer a new RNA strand that can be delivered to a human cell and cause the ribosomes to halt production every time they encounter the coronavirus slippery sequence. This would prevent the virus from replicating in infected people and might cure them. The challenge for the team is to find the right RNA sequence that will affect how the ribosomes respond to SARS-CoV-2 without interfering with the healthy function of the human cell.
“Most antiviral drugs target viral proteins, which we know that viruses are very clever at ‘escaping’ because they can evolve their own proteins quickly. On the other hand, coronavirus is relying on our ribosome to slip through precisely 10 percent of the time. In this case, the virus can’t really do anything about changing our ribosomes because they’re ours. So our idea is to modify our own ribosomes in a way that would only hurt the coronavirus, and we think this strategy could present an insurmountable challenge to the virus.”
When Racism Obstructs Public Health
In more normal times, Alexandre White studies the history of the ways that dynamics of power and politics affect responses to epidemics and pandemics around the world. So when COVID-19 made its appearance, the assistant professor of sociology quickly sought opportunities to help address questions shaping the responses of the present moment.
Working with Lingxin Hao, professor of sociology, and Roland Thorpe, associate professor of health, behavior, and society at the Bloomberg School of Public Health, White applied for a grant from the Hopkins Population Center to use data on demographics and pre-pandemic economic and health factors to better understand unmet health care needs as the virus spread around the country. The three hoped to predict what resources would be needed and where they would be needed most during the virus’s anticipated second wave.
But as the virus raged on, never quite resolving into the expected wave pattern, the team shifted their attention instead toward revealing the underlying causes for the racial disparities that quickly become obvious as COVID-19 struck more Americans of color and made them sicker than white Americans. What they found is that not only do racist policies and structures make Americans of color more likely to have underlying health conditions that put them at greater risk when infected with the virus, but those policies and structures may also mean that they are less able to avoid contact with the virus in the first place.
Plenty was already known about the ways that structural racism is responsible for stark differences in rates and outcomes of many chronic diseases—diabetes, heart disease, and lung cancer, for example—between Black and white Americans. But to understand the intricacies of racism’s impact on COVID in the U.S., White and his colleagues needed to account for the determinants of this disease in particular, such as the way it spreads through close contact with infected people.
“The question of susceptibility, when it comes to being in the same space with the disease, becomes important. We’re looking at the factors that might affect the capacity to safely physically distance.”
Using county-level data showing racial segregation patterns, along with data on virus caseload, White and his colleagues have been exploring how COVID-19-related policy may affect abilities to social distance and how this may be complicated by structural forces of racial discrimination. For example, Black and Latinx Americans are overrepresented in “essential” fields and underrepresented in jobs with the option to work from home, and many rely on public transportation to get to work—all of which places them in contact with many more potentially infected people than workers who stay home. So not only does continued employment put them at greater risk of infection, but when lockdowns are enacted, it becomes harder for them to keep those jobs, and they are typically the first to return when the policies are relaxed.

Racism has significant physiological effects, and the forces of structural racism affect how and to what extent we can protect ourselves from this virus and carry out effective COVID mitigation strategies such as physical distancing and mask wearing.”
—Alexandre White, assistant professor in the Department of Sociology
“These public health recommendations are not necessarily easily adopted or carried out, depending on your economic or social status, and a lot of this has to do with the effects and legacies of racist policies. So one-size-fits-all policies may not affect everyone the same way.”
Instead, White says policymakers should consider employment and transportation factors, along with others including housing, access to services, and living conditions, when devising public health strategies.
“A coordinated federal response to COVID would go a long way,” White adds. “We still lag behind in terms of testing and tracing. We haven’t provided the types of social supports that nations that have been successful in grappling with this have been providing; or effective, cohesive, unified messaging on public health.”